
@ShahidNShah

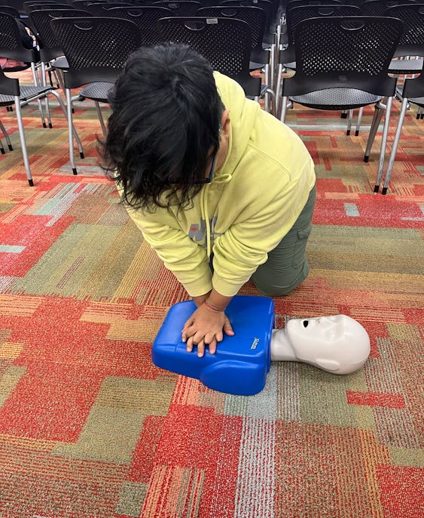
The expectation that only doctors, nurses, and clinical technicians need CPR training is steadily disappearing across the healthcare industry. Hospitals, clinics, dental practices and outpatient centers are quietly extending CPR requirements to receptionists, billing staff, facilities workers and IT teams: anyone who shares a building with patients. The shift isn’t dramatic or sudden, but it’s real, and the reasons behind it are worth understanding for anyone working in a non-clinical role in healthcare or hiring for one.
The most basic reason for the shift is that medical emergencies don’t follow staffing maps. A patient waiting for their appointment can collapse in the lobby. A visitor can suffer a cardiac arrest in a corridor. Someone in the parking garage can have a heart attack on the way out. When that happens, the first person on the scene is rarely a physician; it’s whoever happens to be closest. In a healthcare facility, that’s often a non-clinical staff member whose ability to start chest compressions in the next sixty seconds may be the only thing that matters.
Survival from sudden cardiac arrest depends heavily on what happens in the first four minutes. Brain damage starts at around the four-minute mark without circulation, and survival rates drop roughly ten percent for every minute that passes without CPR. Even inside a hospital, getting a crash cart and clinical team to a patient who’s gone down in a public area can take longer than that. A trained non-clinical staffer can bridge the gap. The presence of CPR-capable people throughout a building dramatically improves the odds for any cardiac event on the premises, regardless of which department it happens in.
The way most healthcare organizations have responded to this is by organizing in-house workplace CPR training for non-clinical departments. Group sessions delivered onsite are now standard at many systems, and the logistics have gotten easier. Training can be scheduled around shifts, certifications are valid for two years, and many providers offer combined CPR and AED sessions in a single half-day. The compliance argument is straightforward, but the practical case is stronger: a workforce where every shift includes multiple CPR-trained people is structurally safer than one where only clinical staff carry the skill.
Joint Commission accreditation standards and state-level healthcare regulations have increasingly favored broader CPR coverage across staff, not narrower. OSHA workplace safety requirements layer in on top of this for facilities employees specifically. Insurance carriers have also started asking pointed questions during liability reviews about how many CPR-trained staff are present on each shift, not just whether the clinical roster is covered. None of these pressures individually mandate non-clinical CPR training, but together they push organizations toward extending it as a baseline rather than treating it as a clinical-only credential.
Beyond what employers organize, non-clinical staff are increasingly pursuing their own credentials, especially as healthcare jobs have become more competitive. A CPR and emergency response certification on a resume signals something employers actually value, particularly for front-desk and patient-facing roles. The broader emergency response training also covers areas basic CPR doesn’t, including choking response, AED operation, bleeding control, and general first aid for the kinds of incidents that happen in waiting rooms. Staff who hold these credentials tend to be more useful in everyday small emergencies, not just cardiac arrests.
The underlying change here is cultural as much as regulatory. Healthcare leadership has moved away from the idea that emergency response is something done by specialists with everyone else getting out of the way. The newer model treats the whole building as a potential response team, with clinical staff leading but non-clinical staff capable of starting interventions and supporting them while the clinical team arrives. This produces better outcomes and a healthier internal culture, where no one in the building has to feel useless during the moments that matter most.
The trend is unlikely to reverse. As regulations tighten and the cost of training drops, the expectation that everyone working in healthcare can perform CPR is going to keep extending outward. For non-clinical staff, getting trained early is increasingly a basic professional move rather than an optional extra.

As Dr. Joel Ross knows all too well, providing ethical, compassionate care is essential to building trust and achieving positive outcomes for patients. In the modern clinical setting, professionals …
Posted May 9, 2026 Personalized Medicine Medicine
Connecting innovation decision makers to authoritative information, institutions, people and insights.
Medigy accurately delivers healthcare and technology information, news and insight from around the world.
Medigy surfaces the world's best crowdsourced health tech offerings with social interactions and peer reviews.
© 2026 Netspective Foundation, Inc. All Rights Reserved.
Built on Jun 3, 2026 at 3:35pm