
@ShahidNShah

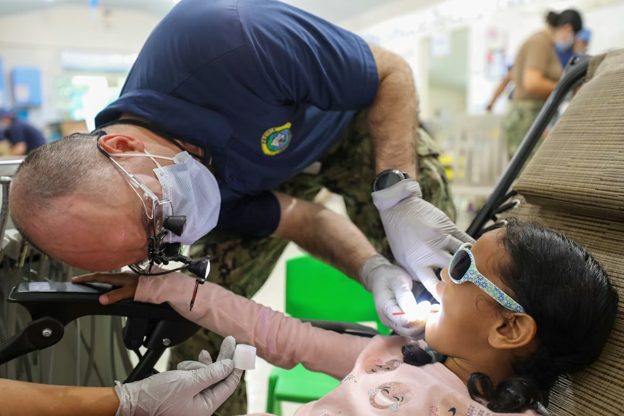
When a seven-year-old needs extensive dental work but freezes with terror at the sight of dental instruments, parents face an impossible choice: force a traumatic experience or delay necessary treatment. According to the American Academy of Pediatric Dentistry’s 2024 guidelines, nearly 20% of children experience severe dental anxiety that interferes with proper oral care. As pediatric dental practices in Sunnyvale increasingly adopt sedation protocols to address this challenge, the conversation has shifted from whether sedation is necessary to how it can be delivered most safely.
The stakes couldn’t be higher for families navigating this decision. Untreated dental problems in children don’t simply resolve on their own — they compound, often requiring more invasive procedures later. Yet sedation carries inherent risks that demand careful consideration and expert management. For parents in the Bay Area, where pediatric dental practices offer varying levels of sedation expertise, understanding the safety protocols and selection criteria has become essential knowledge. The difference between a positive sedation experience and a concerning one often comes down to factors most parents don’t know to evaluate.
The landscape of pediatric dental care has evolved dramatically over the past decade, with sedation becoming a standard tool rather than a last resort. Children today face more complex dental procedures earlier in life, partly due to dietary changes and increased detection of developmental dental issues. Traditional behavior management techniques — tell-show-do methods, distraction, and positive reinforcement — work well for many children, but they have clear limitations when anxiety overwhelms a child’s ability to cooperate.
What makes sedation particularly crucial in modern pediatric dentistry is the recognition that traumatic dental experiences create lasting psychological impacts. Research from the Journal of Pediatric Dentistry shows that children who undergo painful or frightening dental procedures without appropriate anxiety management are significantly more likely to avoid dental care as adults. This avoidance leads to more serious oral health problems later in life, creating a cycle of dental fear and deteriorating oral health.
The COVID-19 pandemic has added another layer of complexity to pediatric dental care. Many children missed routine dental visits during lockdowns, resulting in more advanced decay and the need for more extensive treatment when they finally return to care. Additionally, mask-wearing and social distancing protocols have made traditional comfort measures less effective, pushing more practices toward sedation as a compassionate solution.
In Sunnyvale specifically, the concentration of tech families has created unique demands on pediatric dental practices. Parents often request efficient, comprehensive treatment plans that address multiple issues in single visits, making sedation an attractive option for completing extensive work without multiple appointments. However, this efficiency must never come at the expense of safety protocols designed specifically for children’s developing physiology.
Pediatric sedation operates on a spectrum from minimal relaxation to complete unconsciousness, with each level serving specific treatment needs and patient characteristics. Understanding how these methods work helps parents make informed decisions about their child’s care and set appropriate expectations for the experience.
Nitrous oxide, commonly called laughing gas, represents the mildest form of sedation used in pediatric dentistry. Children inhale a mixture of nitrous oxide and oxygen through a small nasal mask, creating a relaxed, slightly euphoric state within minutes. The child remains awake and responsive throughout the procedure, but anxiety diminishes significantly. What makes nitrous oxide particularly suitable for children is its rapid onset and equally rapid elimination — effects wear off completely within minutes of removing the mask, allowing children to return to normal activities immediately.
Oral conscious sedation involves medications taken by mouth, typically 30-60 minutes before the dental procedure. Common medications include midazolam or hydroxyzine, which create a deeper level of relaxation than nitrous oxide while maintaining the child’s ability to respond to verbal commands. Children under oral sedation often appear drowsy and may not remember the procedure afterward, which can be beneficial for those with severe anxiety. However, the effects last several hours, requiring careful monitoring during recovery.
General anesthesia and IV sedation represent the deepest levels of sedation, reserved for extensive procedures or children with special needs who cannot cooperate under lighter sedation. General anesthesia renders the child completely unconscious, while IV sedation creates a deep sleep-like state with minimal responsiveness. These methods require specialized training, advanced monitoring equipment, and often hospital-based settings due to their complexity and risk profile.
The choice between these options depends on multiple factors: the complexity and duration of the planned procedure, the child’s age and anxiety level, medical history, and the dentist’s training and facility capabilities. A simple cleaning might only require nitrous oxide, while multiple extractions or special needs considerations might necessitate deeper sedation levels.
Safe pediatric sedation relies on rigorous protocols that account for children’s unique physiological responses and potential complications. Unlike adults, children have faster metabolisms, smaller airway passages, and different drug sensitivities that require specialized knowledge and equipment to manage safely.
Comprehensive pre-sedation assessment forms the foundation of safe practice. Qualified providers conduct thorough medical histories, reviewing current medications, allergies, and previous anesthetic experiences. They evaluate the child’s airway anatomy, looking for conditions like enlarged tonsils or unusual facial structures that might complicate breathing during sedation. Weight-based dosing calculations ensure medications are precisely calibrated to the individual child’s needs, avoiding both under-sedation that fails to achieve cooperation and over-sedation that creates unnecessary risks.
Continuous vital sign monitoring during sedation tracks heart rate, blood pressure, oxygen saturation, and respiratory rate throughout the procedure. Pediatric patients require age-appropriate monitoring equipment designed for smaller bodies and different normal ranges. Qualified practices maintain backup monitoring systems and emergency medications specific to pediatric resuscitation protocols. The monitoring doesn’t end when the dental work finishes — recovery monitoring continues until the child meets specific discharge criteria demonstrating full return to baseline function.
Staff training and emergency preparedness separate qualified sedation providers from those attempting to offer services beyond their capabilities. Dentists providing sedation must complete specialized training in pediatric advanced life support (PALS) and maintain current certifications. Support staff receive training in recognizing sedation complications and assisting with emergency protocols. The practice maintains emergency equipment sized for children, including pediatric-sized airway management tools and emergency medications with pre-calculated pediatric dosages.
Facility requirements for safe pediatric sedation include adequate space for monitoring and recovery, suction equipment capable of clearing pediatric airways, and oxygen delivery systems with backup supplies. Many states require specific permits and regular inspections for dental practices offering sedation services, ensuring compliance with safety standards. Access to emergency medical services and clear protocols for transferring patients to hospital care if complications arise complete the safety framework.
The critical difference between safe sedation and dangerous sedation lies in the monitoring protocols and emergency preparedness measures that most parents never see. During sedation, children’s vital signs can change rapidly, and early detection of problems allows for quick intervention before complications become serious.
Modern monitoring equipment designed for pediatric patients provides continuous feedback on the child’s condition. Pulse oximetry measures oxygen levels in the blood, while capnography tracks carbon dioxide levels in exhaled breath — an early indicator of breathing problems. Blood pressure monitoring adapted for small arms ensures cardiovascular stability, while continuous ECG monitoring detects heart rhythm abnormalities that might indicate medication reactions.
Emergency preparedness extends beyond monitoring to include immediate response capabilities. Qualified practices maintain reversal agents for sedation medications, allowing rapid counteraction if over-sedation occurs. Emergency airway management equipment sized for children, including pediatric bag-mask ventilation devices and endotracheal tubes in multiple sizes, ensures providers can maintain breathing if complications develop. Clear emergency protocols designate staff roles and establish communication with emergency medical services, creating seamless escalation paths when needed.
Selecting a pediatric dentist qualified to provide safe sedation requires evaluating credentials, experience, and practice protocols that extend far beyond general dental training. The complexity of pediatric sedation demands specialized expertise that not all dental practices possess, making informed selection crucial for your child’s safety.
Training and certification credentials provide the foundation for safe sedation practice. Board-certified pediatric dentists complete additional years of specialized training in child development, behavior management, and pediatric medical conditions. For sedation specifically, look for providers with formal sedation training through recognized programs and current certifications in pediatric advanced life support. State dental board permits for sedation services indicate compliance with regulatory requirements and regular inspection protocols.
Experience with pediatric sedation matters significantly in managing the nuances of medicating children safely. Ask potential providers about their sedation volume — how many pediatric sedation cases they complete monthly and their experience with your child’s age group. Providers who regularly perform pediatric sedation maintain sharper skills in recognizing and managing complications. Experience with children who have medical conditions similar to your child’s, such as asthma or developmental delays, adds another layer of relevant expertise.
Facility evaluation reveals important safety considerations that impact sedation outcomes. Visit the practice to observe recovery areas designed for children, monitoring equipment appropriate for pediatric patients, and emergency supplies readily accessible. The practice should willingly discuss their emergency protocols and demonstrate familiarity with pediatric resuscitation procedures. Gentle sedation dentistry for kids requires not just technical expertise but also a practice environment designed specifically for children’s unique needs and safety requirements.
Consultation and communication approach indicates how well the provider will partner with you in your child’s care. Qualified providers conduct thorough consultations, explaining sedation options in detail and discussing your child’s specific needs and concerns. They provide clear pre- and post-sedation instructions, outline potential risks and benefits honestly, and encourage questions throughout the process. Red flags include providers who rush through consultations, minimize risk discussions, or seem uncomfortable discussing their qualifications and safety protocols.
Understanding normal recovery patterns and potential complications empowers parents to support their child’s safe return to baseline function while recognizing when professional intervention might be needed. Pediatric sedation recovery follows predictable patterns, but individual children may experience variations that require careful observation.
Common expected effects during recovery include drowsiness, mild confusion, and unsteady coordination that gradually resolve over several hours. Children may experience nausea, particularly with oral sedation medications, though this typically subsides as the medication metabolizes. Emotional lability — sudden crying or unusual clinginess — occurs frequently as children transition between sedated and normal states. These effects are generally temporary and resolve as the sedation medications clear the child’s system.
Monitoring during recovery focuses on ensuring the child’s breathing, circulation, and consciousness return to normal patterns. Check that your child responds appropriately to their name and simple commands, maintains stable breathing without assistance, and shows improving coordination over time. Hydration becomes important once the child is fully awake, but avoid forcing fluids immediately after sedation when nausea risk remains elevated.
Warning signs requiring immediate attention include difficulty breathing, unusual skin color changes, persistent vomiting, or failure to wake up appropriately within the expected timeframe. Allergic reactions, though rare, may manifest as skin rashes, swelling, or breathing difficulties that warrant emergency medical evaluation. Any concerns about your child’s recovery should prompt immediate contact with the dental provider or emergency medical services, depending on severity.
Supporting comfortable recovery involves creating a calm environment where your child can rest safely while sedation effects resolve. Plan for a quiet day following sedation, avoiding activities requiring coordination or judgment until effects fully clear. Follow specific post-sedation instructions regarding food, drink, and activity restrictions. Most children recover completely within 24 hours, returning to normal energy levels and behavior patterns as the medications eliminate from their systems.
The key to successful sedation recovery lies in balancing appropriate vigilance with reasonable expectations, understanding that temporary effects are normal while remaining alert to signs that might indicate complications requiring professional evaluation.

In medicine, patients are often reduced to clinical terms—conditions, diagnoses, treatment plans. But that language rarely captures the full picture of what patients experience or who they are to the …
Posted Apr 15, 2026 Healthcare
Connecting innovation decision makers to authoritative information, institutions, people and insights.
Medigy accurately delivers healthcare and technology information, news and insight from around the world.
Medigy surfaces the world's best crowdsourced health tech offerings with social interactions and peer reviews.
© 2026 Netspective Foundation, Inc. All Rights Reserved.
Built on May 7, 2026 at 5:06am