
@ShahidNShah

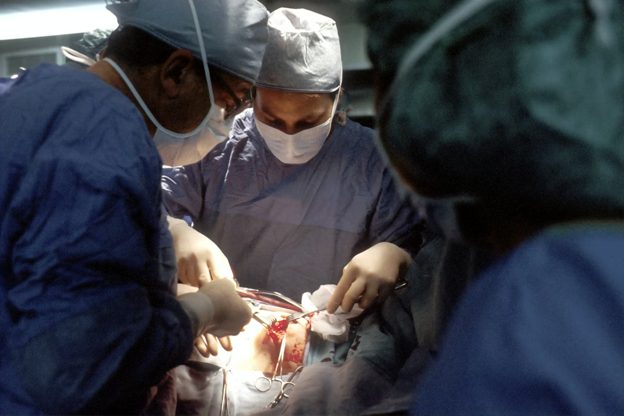
According to the Joint Commission’s 2023 sentinel event data, wrong-site surgeries and retained surgical items account for nearly 15% of all reported preventable medical errors in hospital settings. These incidents represent just the tip of the iceberg in surgical negligence cases — many go unreported or unrecognized until complications become severe. As hospitals nationwide grapple with staffing shortages and increasing surgical volumes, the pressure on operating room teams has intensified, creating conditions where preventable errors become more likely.
For patients and families, recognizing the early warning signs of surgical negligence can mean the difference between addressing problems quickly and facing long-term complications that could have been prevented. The ability to spot these red flags isn’t just about protecting legal rights — it’s about advocating for proper medical care when something goes wrong. Understanding the distinction between negligence and normal surgical risk empowers patients to ask the right questions and seek appropriate intervention when needed.
Surgical procedures inherently carry risks, but negligence occurs when medical professionals deviate from accepted standards of care in ways that harm patients. Unlike other medical errors that might involve miscommunication or administrative mistakes, surgical negligence often happens in real-time during procedures when immediate decisions carry life-altering consequences.
The operating room environment creates unique conditions where negligence can occur. Surgeons work under intense time pressure, often managing multiple complex cases in a single day. Communication failures between surgical team members — anesthesiologists, nurses, and specialists — can lead to critical oversights. When protocols break down or corners get cut to maintain schedule efficiency, patients bear the consequences.
What makes surgical negligence particularly devastating is its immediate and often irreversible nature. A medication error might be caught and corrected within hours, but surgical mistakes like operating on the wrong body part, leaving instruments inside patients, or damaging healthy organs during procedures create complications that require additional surgeries, extended recovery periods, and sometimes permanent disability.
The distinction between unavoidable surgical complications and preventable negligence often hinges on whether established safety protocols were followed. Modern surgery has developed comprehensive checklists, verification procedures, and team communication standards specifically designed to prevent errors. When these systems fail due to human oversight, inadequate training, or institutional pressure to rush procedures, what should have been routine surgery becomes a negligence case.
The financial and emotional toll extends far beyond the initial procedure. Patients may require corrective surgeries, extended hospital stays, rehabilitation, and long-term care for complications that shouldn’t have occurred. For healthcare systems already strained by capacity issues, surgical negligence creates a cascade of additional costs and liability exposure that ultimately affects all patients.
Several indicators during surgery itself can signal that negligence is occurring, though patients are typically unconscious and rely on family members or advocates to recognize these warning signs. Unusual delays or extended surgical times beyond what was initially discussed often indicate complications that shouldn’t be happening. When procedures take significantly longer than scheduled without clear explanation, it may suggest the surgical team is addressing errors or unexpected problems caused by technique failures.
Communication breakdowns among surgical team members create visible tension and confusion in operating rooms. Family members who observe preparation areas or recovery transitions might notice heated discussions, repeated verification procedures, or team members appearing uncertain about next steps. These behaviors often indicate that something has gone wrong or that protocols weren’t properly followed from the start.
Equipment malfunctions or shortages during surgery can force teams to improvise in ways that increase negligence risk. When surgical instruments aren’t working properly or the team lacks appropriate tools for the specific procedure, the likelihood of errors increases dramatically. Patients’ families should be concerned if they hear discussions about equipment problems or see multiple team members leaving to locate alternative instruments.
Post-operative warning signs often provide the clearest evidence that surgical negligence occurred. Unexpected severe pain that doesn’t respond to prescribed pain management suggests potential internal complications from surgical errors. While all surgery involves discomfort, pain that increases rather than gradually improves, or pain in areas unrelated to the surgical site, often indicates problems like nerve damage, infection from poor sterile technique, or retained surgical materials.
Infections that develop unusually quickly or resist standard antibiotic treatment frequently result from contamination during surgery. Surgical site infections should be relatively rare with proper sterile procedures, and when they occur repeatedly or involve unusual bacterial strains, it suggests inadequate infection control protocols during the operation.
Functional problems that weren’t discussed as potential risks before surgery often indicate negligence. When patients lose mobility, sensation, or organ function that should have been preserved during the procedure, it suggests surgical technique errors or damage to structures that should have been protected. These complications require immediate medical attention and thorough documentation for potential nurse negligence claims in Texas or other legal considerations, particularly when post-operative care fails to meet appropriate standards.
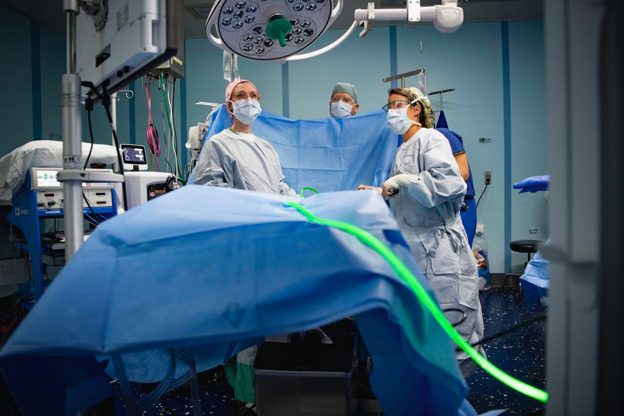
Understanding why surgical negligence occurs requires examining both systemic healthcare problems and individual decision-making failures. Fatigue and overwork among surgical teams creates conditions where even experienced professionals make critical errors. Surgeons often work 12-16 hour days, moving between complex procedures without adequate rest breaks. This exhaustion affects fine motor control, decision-making speed, and attention to detail — all crucial for surgical precision.
Inadequate preoperative planning contributes significantly to preventable errors. When surgical teams don’t thoroughly review patient history, imaging results, or potential complications before procedures begin, they enter operating rooms unprepared for challenges that should have been anticipated. This lack of preparation forces real-time problem-solving that increases error probability.
Communication failures between departments create information gaps that lead to surgical mistakes. When laboratory results, radiology findings, or medication information doesn’t reach surgical teams promptly, they may proceed with incomplete or outdated patient data. These information breakdowns often occur during shift changes or when multiple specialists are involved in patient care.
Institutional pressure to maintain surgical schedules creates environments where safety protocols get abbreviated or skipped entirely. Hospitals facing financial pressure may push surgical teams to complete more procedures in less time, leading to rushed preoperative checks, abbreviated safety discussions, and corner-cutting during procedures. This pressure particularly affects teaching hospitals where residents and medical students may feel compelled to work beyond their skill levels.
Technology integration problems in modern operating rooms can paradoxically increase error rates when staff aren’t properly trained on new equipment or when systems fail during critical moments. Electronic health records, robotic surgical systems, and digital imaging all require extensive training and backup protocols that many healthcare institutions struggle to maintain effectively.
Evidence-based prevention strategies focus on standardizing procedures and improving team communication. Surgical safety checklists have proven remarkably effective at reducing errors when implemented consistently. The World Health Organization’s surgical checklist requires verification of patient identity, surgical site marking, equipment availability, and team introductions before any incision occurs. Research shows these simple protocols can reduce surgical complications by up to 35% when followed religiously.
Time-out procedures before beginning surgery create mandatory pause moments where entire surgical teams verify they’re performing the correct procedure on the right patient at the proper anatomical site. These verification steps catch identification errors, wrong-site surgeries, and procedural confusion before irreversible mistakes occur. Effective time-outs require participation from every team member and cannot be rushed regardless of schedule pressure.
Standardized handoff communication protocols ensure critical information transfers accurately between care teams during shift changes and patient transitions. SBAR communication (Situation, Background, Assessment, Recommendation) provides structured frameworks for sharing patient information that reduce misunderstandings and information gaps that contribute to errors.
Continuing education and simulation training help surgical teams practice managing complications and emergencies in controlled environments. Regular skills assessment and team-based training scenarios allow healthcare professionals to identify knowledge gaps and practice coordinated responses to various surgical challenges without putting actual patients at risk.
Peer review and quality improvement programs create systems for analyzing surgical outcomes and identifying patterns that suggest systemic problems. When hospitals track complication rates, near-miss incidents, and patient feedback systematically, they can implement targeted improvements before errors result in patient harm.
Modern healthcare technology offers powerful tools for preventing surgical negligence when implemented thoughtfully. Electronic health records provide comprehensive patient information access that helps surgical teams identify allergies, medication interactions, and previous surgical history that affects current procedures. However, these systems only prevent errors when information is accurately entered and regularly updated by all healthcare providers involved in patient care.
Barcode scanning systems for patient identification, medication administration, and surgical instrument tracking create multiple verification points that catch errors before they reach patients. These technologies work particularly well for preventing wrong-patient procedures and ensuring proper sterile instrument processing between surgeries.
Patient engagement in safety protocols provides additional error-prevention layers that complement technological solutions. Educated patients who understand their procedures can verify surgical sites, confirm their identity, and speak up when something seems incorrect. This patient involvement requires healthcare teams to explain procedures clearly and create environments where patients feel comfortable asking questions or expressing concerns.
Surgical robotics and computer-assisted procedures can reduce certain types of human error while introducing new technological risks that require different prevention strategies. Teams using these advanced systems need extensive training not just on normal operations but also on managing equipment failures and emergency situations when technology doesn’t function as expected.
Real-time monitoring systems that track vital signs, surgical progress, and equipment function can alert teams to developing problems before they become critical. These early warning systems work best when integrated with established response protocols and team communication strategies that ensure appropriate action gets taken when alerts occur.
The evolution toward more transparent, patient-centered surgical care creates opportunities for families and patients to participate actively in safety verification while building trust between healthcare teams and those they serve. This collaborative approach acknowledges that preventing surgical negligence requires vigilance from everyone involved in the surgical process, not just medical professionals.

According to the American Dental Association’s 2024 oral health surveillance data, over 90% of adults have experienced tooth decay, yet many put off restorative treatment until pain forces their …
Posted Apr 8, 2026 Dental Care Dentistry
Connecting innovation decision makers to authoritative information, institutions, people and insights.
Medigy accurately delivers healthcare and technology information, news and insight from around the world.
Medigy surfaces the world's best crowdsourced health tech offerings with social interactions and peer reviews.
© 2026 Netspective Foundation, Inc. All Rights Reserved.
Built on Apr 8, 2026 at 1:06pm